Birth Control Pills: The Ultimate Guide. Usually, hormone replacement therapy is prescribed once you. For specific hormone levels, see our Hormone Testing helpsheet. Because women going through POF or EM still get their periods sometimes . But on the whole, there seems to be little debate about its use for younger women, that is, women with premature ovarian failure (POF) or early menopause (EM) who are not producing the usual levels of hormones for their age. But what about perimenopause?
But let’s look a little closer at the claim that hormones in birth control are getting into the environment through lady pee.
- Progestin-Only Birth Control: Pill and Injection, an ACOG patient education FAQ, covers progestin-only birth control methods.
- Hormonal methods of birth control come in many forms such as a patch, shot, ring, implant, or birth control pills. Schedule an appointment today at Women’s.
- Is the Birth Control Patch Right for Me? Here are some of the most common questions we hear women ask about the birth control patch. We hope you find the answers helpful.
- Learn about CombiPatch, a hormone therapy that combines estrogen and progestin in a twice-weekly patch.
- The birth control pill was first introduced to the American public for contraceptive use in 1960. By 2002, 11.6 million US women were on 'the Pill.
Hormonal methods of birth control. INTRODUCTIONHormonal methods of birth control contain estrogen and progestin, or progestin only, and are a safe and reliable way to prevent pregnancy for most women.
There are several ways that the hormone(s) can be delivered. Nonhormonal methods, such as the copper IUD and barrier methods, are discussed separately.
The best method is one that will be used consistently, is acceptable to the woman and her partner, and which does not cause bothersome side effects. Other factors to consider include. Each woman must balance the advantages of each method against the disadvantages and decide which method she prefers.
You can get these birth control methods by prescription from your own doctor or from a doctor in a sexual health clinic. The birth control patch is a hormonal contraception. It is a small square patch that looks like a band-aid. It sticks to the skin and releases hormones.
A list of questions that are useful for defining a person's preferences are provided in the table (table 1). BIRTH CONTROL PILLSMost oral contraceptives, also referred to as . The combination pill reduces the risk of pregnancy by.
Although the failure rate is 0. Missed pills are a common cause of pregnancy.
In general, an active pill should be taken as soon as possible after a pill has been missed. Backup birth control should be used for seven days if more than two pills are missed. Side effects — Possible side effects of the pill include.
This is particularly common during the first few months of taking oral contraceptives. This almost always resolves without any treatment within two to three months. Forgetting a pill can also cause breakthrough bleeding. Women taking the pill should notify their healthcare provider if they experience abdominal pain, chest pain, severe headaches, eye problems, or severe leg pain as these could be symptoms of several serious conditions including heart attack, blood clot, stroke, liver, and gallbladder disease. Complications — When the pill was first introduced in the 1. Because of this, cardiovascular complications occurred, such as high blood pressure, heart attacks, strokes, and blood clots in the legs and lungs. Reduced doses of progestin and estrogen in the currently available oral contraceptives have decreased these complications.
Therefore, birth control pills are now considered a reliable and safe option for most healthy, non- smoking women. Blood clots occur in approximately 4 to 1. This compares to approximately 2 to 5 blood clots per 1.
Older age and obesity are major risk factors for developing a blood clot whether or not the woman is taking birth control pills. The majority of studies suggest that taking (or previously taking) the pill does not increase the risk of breast cancer. Who should not take the pill? Women with diabetes and vascular complications from diabetes should not use the pill. Medication interactions — The effectiveness of the pill may be reduced in women who take certain medications. Anticonvulsants — Some anticonvulsants, including phenytoin (Dilantin), carbamazepine (Tegretol), barbiturates, primidone (Mysoline), topiramate (Topamax) and oxcarbazepine (Trileptal) decrease the effectiveness of hormonal birth control methods (pill, patch, ring).
As a result, women who take these anticonvulsants are advised to avoid hormonal birth control methods (with the exception of depo- medroxyprogesterone acetate . However, there is some concern that oral contraceptives may reduce the effectiveness of lamotrigine, potentially increasing the risk of seizures. Antibiotics — Rifampin, which is sometimes used to treat tuberculosis, can decrease the efficacy of hormonal birth control.
As a result, women who take rifampin should not use any hormonal birth control method (pill, patch, ring, implant, injection). Other methods (condom, diaphragm, IUD, sterilization) are recommended. Other antibiotics (eg, penicillin, tetracycline, cephalexin) do not affect the efficacy of hormonal birth control methods. Back- up contraception is not needed when you take these antibiotics. St. John's wort, an herbal supplement sometimes taken to treat depression, may reduce the effectiveness of birth control pills.
A back- up form of birth control (eg, condoms) is needed for the first seven days after the quick start. Many women start their pill on the first Sunday after the period starts (because most pill packs are arranged for a Sunday start). Some form of back- up contraception is needed for the first seven days after the Sunday start. When to expect a period — Traditionally, the pill is taken on a 2. Some newer formulations have a longer duration of hormone pills and fewer days of placebo pills (eg, 2. It is not necessary to take the placebo pills, but some women find it easier to remember to start their next pill pack if they have taken the placebos. The period should occur during the fourth week of the pill pack, ie, the .
This allows them to have fewer days of menstrual bleeding per year. This regimen is a particularly good treatment for women with painful periods or endometriosis, as well as those who want to avoid a monthly bleed. Traditional birth control pill packs can be used in continuous dosing. In this regimen, the woman takes the first three weeks of a pill pack, then immediately starts a new pack (without a break); the last week of (placebo) pills is not used.
This can be continued for as long as desired. Seasonale is an extended cycle birth control regimen in which an active pill is taken every day for 1. Seasonique is another extended cycle pill that contains seven days of a low dose estrogen pills instead of the placebo pills; this is intended to reduce breakthrough bleeding and estrogen withdrawal symptoms.
Taking an oral contraceptive for an extended time results in fewer periods per year, although many women experience breakthrough bleeding when starting this regimen. Breakthrough bleeding is inconvenient, but does not indicate an increased risk of pill failure (unless pills are forgotten). Shorter pill- free interval — Several pill formulations are available with 2. It is hoped that pill failures and side effects will be minimized with this approach.
Progestin only pills — Some pills contain only progestin (called the mini pill), which is useful for women who cannot or should not take estrogen. This includes women who are breastfeeding and within 4 to 6 weeks of delivery or who have worsened migraines or high blood pressure with combination contraceptive pills. Progestin only pills are as effective as combination pills when taken at the same time every day, but there is a slightly higher failure rate of the mini pill if the woman is more than three hours late in taking it. A back up method of birth control should be used for seven days if a pill is forgotten or taken more than three hours late. Progestin only pills are taken on a 2.
One pill should be taken every day at the same time, and there is no placebo pill week. Breakthrough bleeding or spotting can occur with progestin only pills. Emergency contraception — If you have sex and have forgotten to take your pill, patch, or vaginal ring, or you are more than two weeks late for your injection of medroxyprogesterone acetate, you can take a .
This should be taken as soon as possible after sex, ideally within 1. DMPA is injected deep into a muscle, such as the buttock or upper arm, once every three months.
A preparation that is given subcutaneously (under the skin) is also available. DMPA prevents ovulation and thickens the cervical mucus, making the cervix impenetrable to sperm.
If the first dose of DMPA is given during the first seven days of the menstrual period, it prevents pregnancy immediately. A woman who receives her first DMPA injection after the seventh day of her period should use a second form of contraception (eg, condoms) for seven days.
DMPA is very effective, with a failure (pregnancy) rate of less than one percent when the injection is given on time. Side effects — The most common side effects of DMPA are irregular or prolonged bleeding and spotting, particularly during the first few months of use. Up to 5. 0 percent of women completely stop having menstrual periods (amenorrhea) after one year of DMPA use. Menses generally return within six months of the last DMPA injection. DMPA is associated with weight gain in some women.
In women who use injectable progestins, there is no increased risk of cardiovascular complications or cancer. Use of DMPA is associated with decreased bone mineral density in current users. This effect is mostly reversed after DMPA is stopped.
Studies have not shown an increased risk of bone fractures in women who have used DMPA in the past. Because DMPA is long- acting, it may not be ideal for women who wish to become pregnant shortly after stopping the medication. Although most women are able to conceive within 1. There are a number of women who prefer DMPA to the pill, including those who. The patch is as effective as oral contraceptives, and may be preferred by some women because it does not require daily dosing. However, the failure rate of the patch is higher for obese women (eg, who weigh more than 1.
Xulane is the only skin patch contraceptive available in the United States. Effectiveness is similar to that of oral contraceptive pills. However, the patch may deliver a higher overall dose of estrogen than the pill.
Some studies found that this was associated with an approximate doubling of the risk of blood clots while others found no increase in risk. Further study is needed to define this risk.
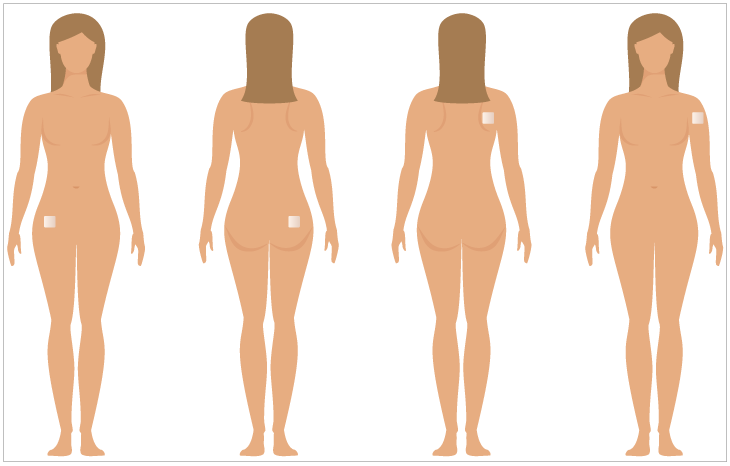
The patch is worn for one week on the upper arm, shoulder, upper back, abdomen, or buttock (picture 1). After one week, the old patch is removed and a new patch is applied; this is done for three weeks. During the fourth week, no patch is worn; the menstrual period occurs during this week. VAGINAL RINGNuvaring is a flexible plastic vaginal ring that contains estrogen and a progestin, which is slowly absorbed through the vaginal tissues (picture 2. A- B). This prevents pregnancy, similar to an oral contraceptive. It is worn in the vagina for three weeks, followed by one week when no ring is used; a menstrual period occurs during this time.
The ring's position inside the vagina is not important.
 RSS Feed
RSS Feed
